Skin Cancer Treatments
About Mohs Micrographic Surgery
Pioneered over 70 years ago by Dr. Frederic E. Mohs, Mohs micrographic surgery is a state-of-the-art procedure that has undergone significant refinements both in diagnostic pathology and plastic surgery reconstruction. With the Mohs technique, our Mohs surgeon is able to see beyond the visible disease, to precisely identify and remove the entire tumor layer by layer while leaving the surrounding healthy tissue intact and unharmed. As the most exact and precise method of tumor removal, it minimizes the chance of re-growth and lessens the potential for scarring or disfigurement.

Dr. Julia Arzeno, MD, FAAD
Mohs Micrographic Surgeon, Board Certified Dermatologist
Seeking the best in skin cancer treatment in the Bay Area? Meet Dr. Julia Arzeno, MD, FAAD, Berman Skin Institute’s leading Mohs Micrographic Surgeon. Serving patients at our Walnut Creek and Pleasanton locations, Dr. Arzeno brings specialized training and a proven track record of over 2,000 successful Mohs surgeries. Her commitment to precise, tissue-sparing techniques ensures the most effective skin cancer removal with exceptional cosmetic results.
Choose a reason for your visit:
Because our Mohs surgeon has specialized fellowship training in dermatologic oncology, pathology, and plastic surgery reconstruction, the Mohs procedure has the highest cure rate of all treatments for skin cancer – up to 99%. Mohs surgery is the gold-standard treatment of choice for cancers of the face and other cosmetically-sensitive areas as it utilizes precise microscopic examination to trace the edges of the cancer and thus ensure its complete removal.
Treatment Videos
Benefits of Mohs Micrographic Surgery
Mohs micrographic surgery is an effective and precise method for curing basal cell and squamous cell skin cancers as well as several other, less common skin cancers. Because Mohs micrographic surgery uses a systematic microscopic process that traces skin cancer down to its roots, it offers the highest chance for complete removal of the tumor while sparing the normal tissue surrounding it.
Clinical studies conducted at various national and international medical institutions – including the Mayo Clinic, the University of Miami School of Medicine and Royal Perth Hospital in Australia – demonstrate that Mohs surgery provides five-year cure rates exceed 99 percent for new cancers, and 95 percent for recurrent cancers.
How Does Mohs Surgery Work?
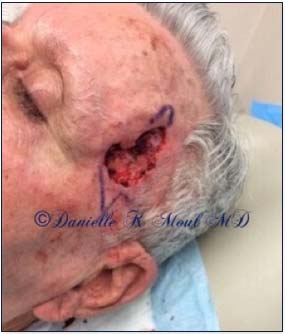
Skin tumors are removed one layer at a time and frozen sections are examined under the microscope immediately after they are removed. Using the microscope, our Mohs surgeon can see which way the tumor is growing. Often, these tumors grow like roots of a tree, extending farther under normal-looking skin than what you see with the naked eye.
While the patient relaxes in the waiting room, the tissue is examined. The frozen section tissue processing and microscopic examination of the lesion between stages requires 45 minutes to an hour. During this time, the patient will be allowed to sit in the waiting room with friends or family. We recommend bringing ample reading material (books, magazines, laptop computer, etc.) and plenty of food to snack on. We will provide a quiet, peaceful environment and beverages such as coffee, tea and water.
The patient reenters the treatment room and additional tissue is removed only in the area where the margin was positive. Most cases are cleared in one to three stages; however, larger or recurrent tumors often require multiple stages. The tumor removal and reconstructive surgery typically occurs in a single day, requiring approximately five to eight hours from beginning to end. If the patient is scheduled for a 9:00am surgery start time, he or she should not expect to leave the surgery center until approximately 12 – 4pm.
Occasionally, complex cases require more time and / or delayed reconstructive repairs. In such cases, we will meet with you to discuss these issues and answer any questions or concerns.
Who is a Candidate?
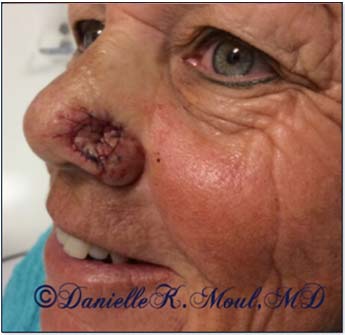
Mohs surgery is indicated for any skin cancer in a cosmetically-sensitive area of the head and neck (i.e. ear, lip, nose, cheek, temple, eyelid, forehead, chin, scalp, etc.) and rare or large skin cancers of the body and extremities. Individuals of any age may develop skin cancer, although most are over age 40. Skin cancer may occur in any skin color, although red-heads and fair Caucasian skin types are at highest risk.
What Can I Expect During Mohs Micrographic Surgery?
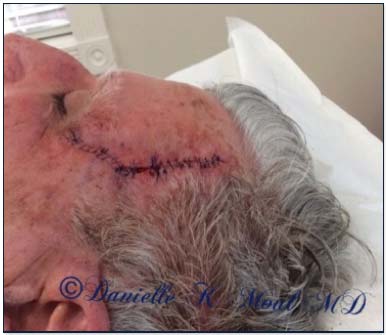
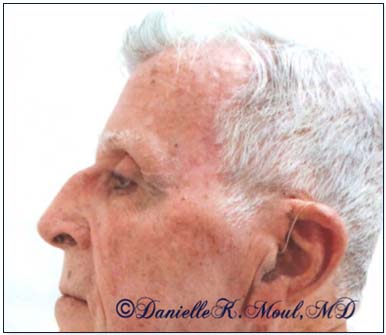
Our Mohs surgeon has extensive training in reconstructive procedures and often performs the wound closure after the tumor is removed. A small wound may be allowed to heal on its own, or the wound may be closed with stitches, a skin graft or a flap. Since Mohs surgery preserves the maximum amount of normal skin, this results in smaller scars. Repairs are more often simple and involve fewer complicated reconstructive procedures.
If a tumor is larger than anticipated, another surgical specialist with unique skills may complete the reconstruction. In this situation, the patient may be sent home with a special bandage until the following day or may go directly to the specialist immediately following the tumor removal. Every effort will be made to anticipate these more complex situations and a consultation with our Mohs surgeon will be scheduled prior to the Mohs surgery day.
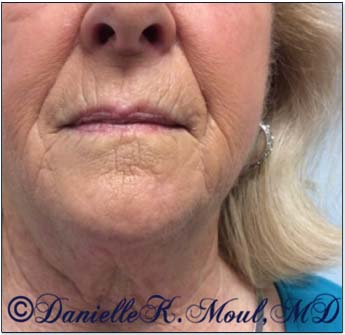
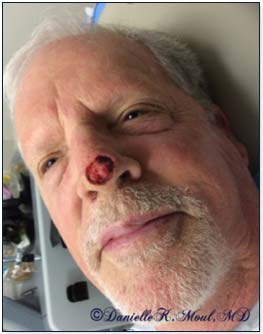
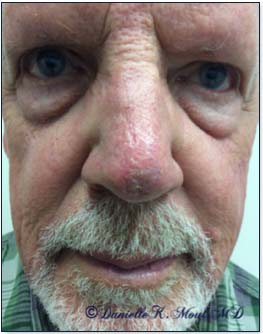
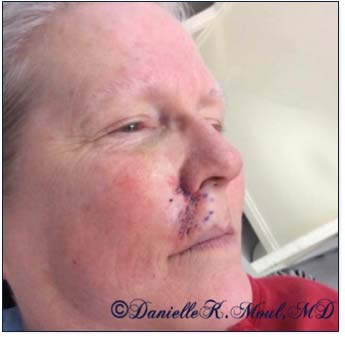
Results may vary.
Does Mohs Surgery Hurt?
Your skin will need to be numbed with a needle. This will hurt for several seconds before the area becomes numb. However, you may request numbing cream ahead of time which will dull the needle prick. If you have a ride home, we can also give you some oral sedatives and pain medication. The majority of patients do not need this type of medication. After the procedure, the area that was operated on will be sore. Usually, Tylenol Extra Strength will decrease the discomfort. Ice or cold packs in the area—20 minutes per hour while you are awake will also help.
What Safety & Side Effects Are There for Mohs Surgery?
Because only local anesthesia is used (injection into skin), the risks associated with general anesthesia are eliminated. Occasionally, mild sedatives will be provided, such as Valium or Ativan, and the patient will require someone to drive them home. Expected side effects are wound tenderness, bruising and swelling. Swelling may persist one or two weeks after surgery, especially if the tumor is located on the eyelid, nose or cheek. Rare complications include bleeding into the wound (hematoma) and infection, both occurring in less than 1% on average. In these cases, the hematoma will be drained and the infection will be treated with antibiotics. Occasionally, our Mohs surgeon will find it prudent to provide prophylactic antibiotics for the patient, especially if the patient has a history of heart valve or joint replacement, immune suppression, history of infection or a blood clotting disorder.
What is the Recovery Time for Mohs?
If the reconstruction is on the head and neck, Dr.Berman will (in most patients) put in all absorbable stitches. The skin stitches will dissolve in 7-10 days and don’t need to be removed. There is no suture removal. The deep sititches may take several months to absorb. If our Mohs surgeon has used a skin graft to repair the wound, then you will need to return in one week to remove the dressing. On the rest of the body, our Mohs surgeon will use nylon sittiches in the top layer of the skin, and these stitches are generally removed in two weeks. Bruising and swelling may last 2-3 weeks.
What Should I Do Before Mohs Surgery?
Continue taking your usual medications, even on the day of surgery, unless you are directed by a physician. You will be asked to inform our Mohs surgeon whether you are taking any blood-thinning medications such as warfarin, Plavix, aspirin, ibuprofen, vitamin E, or others. Blood-thinners can lead to increased bleeding, swelling and bruising following surgery.
Please get a good night’s rest and eat normally prior to your surgery. It is important that you bring healthy snacks and a sack lunch on the day of your surgery. We recommend that you wear comfortable clothing and an extra layer for warmth. Please wear a shirt that can be removed without pulling it over your head (i.e. one with buttons or zippers down the front). A book, magazine, or laptop computer may be helpful during the waiting periods of the day. Also, you may want to arrange for a friend or family member to drive your home. You will not be allowed sedatives or strong pain medication during surgery if you are planning to drive yourself home.
What Should I Do After Mohs Surgery?
Post-operative wound care instructions are reviewed with the patient and patient’s family and / or surgery-day companion by the Mohs surgical nurse and a thorough wound-care instruction form is provided, along with our Mohs surgeon’s cell phone number in case of questions that may arise in the evenings or over the weekend.
A bandage will be placed on your wound. This bandage will remain on the wound for 2 days (unless it is a graft, then it is for a full week), then you will need to start changing it daily for two weeks. You will be given wound care instructions and the staff will go over it with you. If our Mohs surgeon stitches your wound, then you will be prescribed antibiotics for 5 days.
Pain after surgery is generally described by patients as “throbbing” or like a “deep bruise” but is not typically sharp in nature. Surgery on the forehead or scalp may trigger headaches on the first night or first few days of recovery. Over-the-counter and / or prescription pain medications may be necessary and will be discussed on the day of surgery.
If you have further questions about the Mohs procedure, please feel free to contact our center. You may also contact the American College of Mohs Micrographic Surgery and Cutaneous Oncology at (800)500-7224 or info@mohscollege.org.
Who Performs Mohs Surgery?
Our Mohs skin cancer surgeon is board-certified by the American Board of Dermatology and is a Fellow of the American College of Mohs Micrographic Surgery.
Alternatives to Mohs Surgery
Alternative treatments to Mohs micrographic surgery for skin cancers of the face do not offer a high cure rate and do not provide the aesthetic surgical outcomes that can be achieved with reconstructive surgery by a fellow-ship-trained Mohs surgeon. For some superficial basal cell carcinomas, simple “scraping and burning” techniques have been used, but the cure rates vary from 50 – 70% at best, and the resulting scars are generally disfiguring. Standard surgical excision offers about 70% cure for the most common types of skin cancers, but the resulting “hole” or surgical defect is typically much larger than that following tumor removal using the Mohs technique. In addition, standard excision is not typically followed by plastic surgery reconstruction since the margins are not known to be clear until the final pathology is reviewed, which may be up to two weeks after the surgery. Mohs surgery is considered the “gold standard” treatment for skin cancers of the head and neck and for large or unusual tumors of the body and extremities.
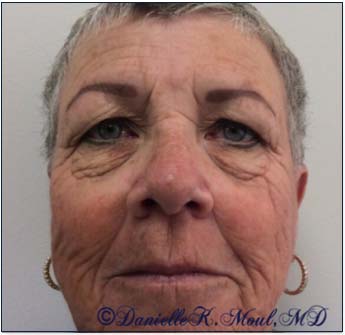
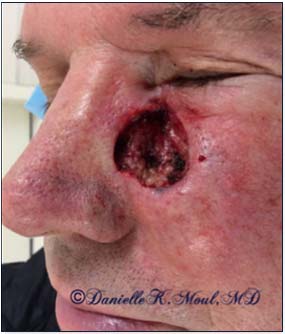
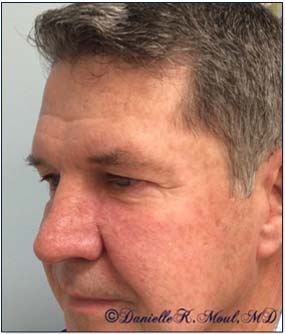
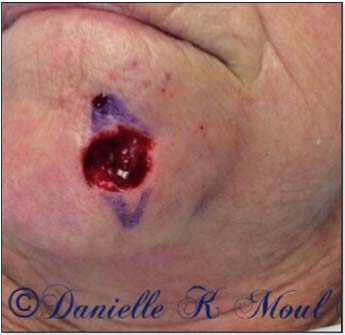
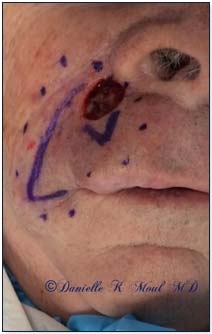
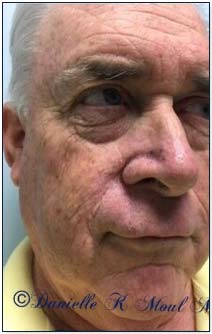
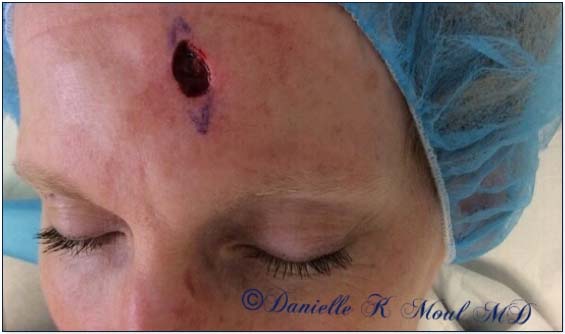
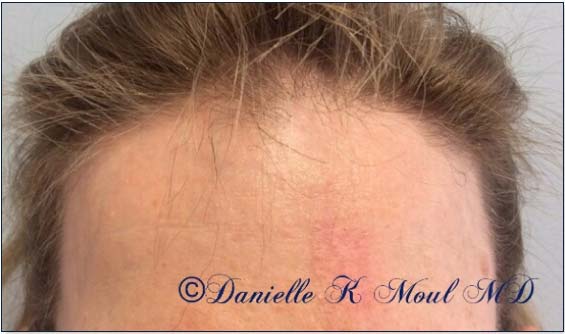
Mohs Gallery
Please select the various patients to view individual results.
*Results may vary.